With support from The Commonwealth Fund, KNG Health estimated the extent to which post-hospital home health (HH) use increased among traditional Medicare beneficiaries during the COVID-19 public health emergency. We found large shifts in hospital discharges toward HH across all groups during 2020 driven, in large part, by reductions in discharges to skilled nursing facilities (SNFs).
As a lower cost setting, the increased use of HH may drive Medicare program savings but with uncertain impact on outcomes. To begin to understand the potential impact of shifting post-acute care patterns, we assessed changes in hospital discharge volume to HH and SNFs by Medicare-Severity Diagnosis Related Group (MS-DRG) and patient complexity between October 2019-February 2020 and March 2020-December 2020 for the MS-DRGs with the highest HH volume prior to COVID-19. We use the period from October 2019 through February 2020 as our pre-COVID-19 baseline, because a new Medicare payment system for SNFs was implemented on October 1, 2019. To measure patient complexity, we mapped the comorbidities and complications (CCs) and major CCs (MCCs) lists created by the Centers for Medicare & Medicaid Services to a patient’s hospital claim and counted the number of CCs and MCCs.
Home health’s share of discharges increased 4 to 9 percentage points among the top 25 MS-DRGs determined based on HH volume, including septicemia or severe sepsis, major hip and knee joint replacement, heart failure and shock. The corresponding decreases in the SNF share ranged from 2 to 13 percentage points. After stratifying by complexity, we generally found increases in HH use and decreases in SNF use across all complexity categories. Further, for many of the MS-DRGs examined (20 MS-DRGs out of the top 25), we observed a larger shift toward HH among more complex cases. For example, looking at patients with major hip and knee joint replacement or reattachment of lower extremity without MCC (MS-DRG 470), HH’s share of patients has increased 6 percentage points for those with fewer than 3 CCs. In contrast, HH’s share of patients with 6 or more CCs increased by 9 percentage points. The corresponding decrease in SNF’s share was 4 and 10 percentage points, respectively.
To better understand the implications of this shift on the Medicare population, we are examining the extent of the shift for several sub-populations: Black beneficiaries, dual eligible, high-cost, and high-needs patients. We are also analyzing health outcomes and Medicare spending associated with the abrupt shift in PAC use observed during the COVID-19 public health emergency.
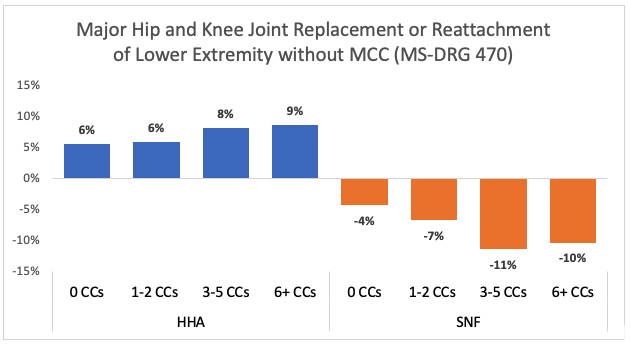
Note: HHA – Home Health Agency; SNF – Skilled Nursing Facility; CC – Comorbidities and Complications; MCC – Major Comorbidities and Complications