Over the past year, the COVID-19 pandemic has ravaged the country and overwhelmed the U.S. healthcare system with overflowing intensive care units (ICUs) and overworked medical professionals. Although short-term acute care hospitals (STACHs) are the nation’s frontline in treating severe COVID-19 cases, the post-acute care (PAC) sector—home health agencies (HHAs), skilled nursing facilities (SNFs), inpatient rehabilitation facilities (IRFs), and long term care hospitals (LTCHs)—has played an important supporting role. Early on in the pandemic, some advocated for an expanded role for LTCHs and SNFs to aid in the response to the pandemic, while others noted that limits in institutional PAC capacity would potentially require greater use of HHAs to address the pandemic. Now, a year into the public health emergency, an examination of Medicare claims data confirms the role that the PAC sector played during the initial months of the nation’s COVID-19 response.
Medicare Post-Acute Care Patterns Shifted Under COVID-19 Pandemic Relative to 2019
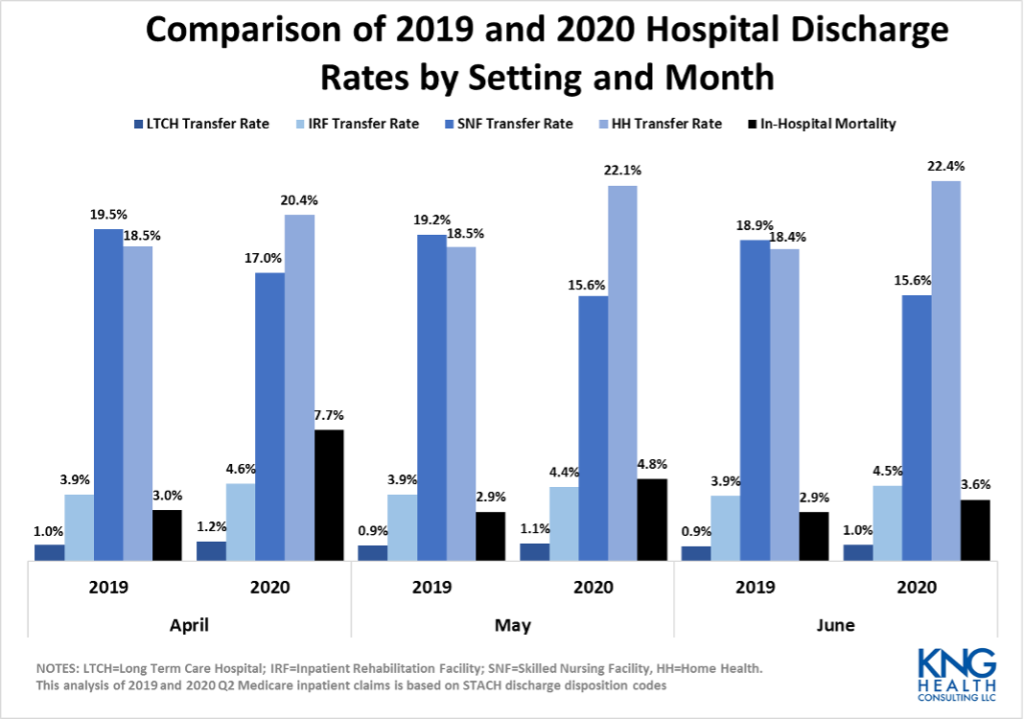
Medicare fee-for-service (FFS) claims data from the first wave of the pandemic (April 2020-June 2020) indicate that PAC utilization patterns shifted, in terms of the distribution of patients across PAC settings and patient mix. Despite an overall decrease in PAC volume, compared to the previous year, the percent of patients transferred from a STACH to a PAC setting increased in the second quarter of 2020. However, a smaller share of STACH patients was transferred to SNFs relative to 2019, while a significantly greater share was discharged with a home health referral. In addition, the transfer rate to LTCHs was almost 4 times higher for COVID-19 patients than non-COVID-19 patients in June 2020. While COVID-19 patients were also more likely to transfer to a SNF than non-COVID-19 patients (twice as likely in June 2020), the opposite is true for patients transferred to an IRF or HHA.
Between April and June 2020, Medicare Volume Was Down and Patient Complexity Was Up in PAC
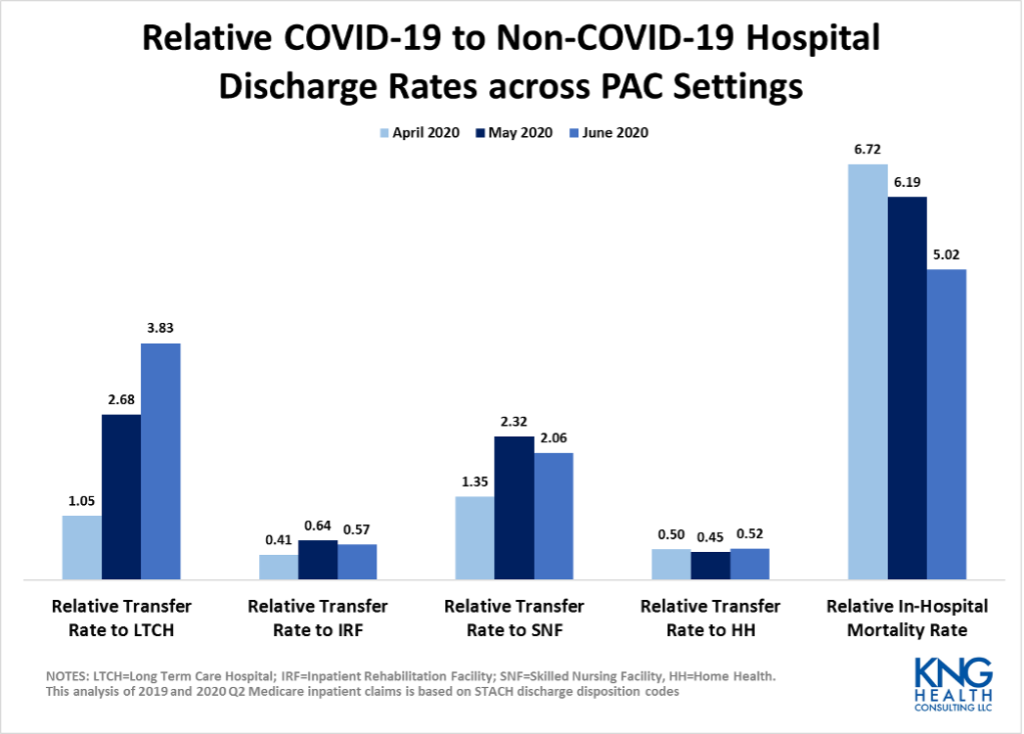
LTCHs and SNFs Shifted their Focus to COVID-19 Patients
The transfer rate of COVID-19 cases to LTCHs and SNFs was significantly higher than for non-COVID-19 cases. In June 2020, a Medicare beneficiary with COVID-19 was almost 4 times more likely to go to an LTCH than a non-COVID-19 patient. During the same period, COVID-19 patients were twice as likely to go to a SNF as non-COVID-19 patients. In contrast, COVID-19 patients were roughly half as likely to go to an IRF or HHA as non-COVID-19 patients. The large differential in likelihood of transferring to an LTCH between COVID-19 and non-COVID-19 patients demonstrates the significant role these specialty hospitals have played during the public health emergency.
Future Work Needed to Gain a Deeper Understanding of PAC Role in COVID-19 Pandemic
At the beginning of the pandemic, the Centers for Medicare & Medicaid Services (CMS) instituted a number of waivers for PAC providers that provided some needed flexibility in responding to the needs of their communities. While our findings should be considered preliminary because it is based on an early release of Medicare claims data, our findings suggest that the waivers had the intended effect of allowing PAC providers to address the pandemic more easily.
Once we get past the acute phase of the pandemic, there will undoubtedly be a thorough assessment of where the U.S. healthcare system succeeded and struggled, with identification of ways to improve the effectiveness and equity of our care delivery systems. That work should include an assessment of PAC. Understanding PAC utilization patterns during the public health emergency may help shed light on the roles of these different PAC providers in caring for Medicare beneficiaries and how those roles can be improved going forward.
[1] Medicare Payment Advisory Commission. A Data Book: Health Care Spending and the Medicare Program. July 2020. Chapter 8 accessed at http://medpac.gov/docs/default-source/data-book/july2020_databook_sec8_v2_sec.pdf?sfvrsn=0
Services : Blog, Practice Area - Evaluation and Health Economics Expertise: COVID-19, Healthcare Cost and Utilization, Medicare, PAC, post-acute care